T1International in Kenya: Part 1
12 May 2016, 9:40 p.m. in Global Stories, News & Statements by Elizabeth Pfiester
T1International recently had the opportunity to visit Kenya, supporting an NCD Child Advocacy workshop in the town of Eldoret. While there, we visited the diabetes clinic and then headed to Nairobi to spend some time with our type 1 Global Advocate, Mbolonzi. Mbolonzi runs a nonprofit called Diabetes Awareness Prevention and Management Kenya and we were lucky to join their meet up for people with diabetes. This series of blog posts will summarize our experience and some highlights of what we learned about advocacy and life with type 1 diabetes in Kenya. We’ll start with the clinic visit to Moi University Teaching Hospital in Eldoret.
 On our first day in Eldoret the diabetes team at Moi University Teaching Hospital, lead by Deborah, gave us a thorough tour of the diabetes clinic there. The center attends to 4,000 diabetes patients, with almost as many patients at satellite clinics. We were able to meet many members of the highly committed diabetes team and, to say the least, we were very inspired by their passion. Deborah showed us the home glucose monitoring clinic, foot clinic, and diabetes education and counselling centre. Patients on clinic days often have to wait for 7 hours to be seen. Despite this, the team does their best to ensure thorough and personal service after the patient has waited so long.
On our first day in Eldoret the diabetes team at Moi University Teaching Hospital, lead by Deborah, gave us a thorough tour of the diabetes clinic there. The center attends to 4,000 diabetes patients, with almost as many patients at satellite clinics. We were able to meet many members of the highly committed diabetes team and, to say the least, we were very inspired by their passion. Deborah showed us the home glucose monitoring clinic, foot clinic, and diabetes education and counselling centre. Patients on clinic days often have to wait for 7 hours to be seen. Despite this, the team does their best to ensure thorough and personal service after the patient has waited so long.
Resources are scarce and it is impossible for many people to afford everything they need to survive with diabetes. The diabetes team are practical and considerate in their education and advice. For example, they tell patients to use syringes 3x each (unless it becomes contaminated or dirty) and to test blood sugars 2x per day when they have very limited strips.
Abbot provides glucometers and test strips for home glucose monitoring. Most patients test twice on 3 days of the week to look for patterns and adjust insulin, rather than once each day which would not tell them anything about the direction of their blood sugar level. The team decided to reduce the number of days of blood sugar monitoring for each patient in order to allow more patients to be able to self monitor. Abbott’s support of the clinic allows people to test their blood sugar when they otherwise would not be able to. Still, patient numbers continue increasing which makes resources stretched.
If not for the free supplies from the clinic, the cost in Kenyan shillings would be:
50 strips: 3000 (30 USD)
Insulin: 800-1400 (8-14 USD)
10 syringes: 30 (3 USD)
Keep in mind a huge portion of the population (more than 40%) lives below the poverty line or survives on minimal income, so these costs would take up a huge portion of that income. The clinic subsidizes costs as much as possible and gets discount bulk rates.
 We met Jemima, a clinician and program lead, who believes strongly in the importance of one-on-one diabetes education to ensure the patients understand their responsibility and feel assured. Jemima is a lovely lady who really cares deeply about her patients. She worked hard to get Eli Lilly to provide insulin by first convincing them providing it for 50 street boys and orphans. She collected case studies and fed them back to Lilly, and secured another 200 vials. The positive outcomes displayed by the clinic have allowed donations of almost enough insulin to cover patients.
We met Jemima, a clinician and program lead, who believes strongly in the importance of one-on-one diabetes education to ensure the patients understand their responsibility and feel assured. Jemima is a lovely lady who really cares deeply about her patients. She worked hard to get Eli Lilly to provide insulin by first convincing them providing it for 50 street boys and orphans. She collected case studies and fed them back to Lilly, and secured another 200 vials. The positive outcomes displayed by the clinic have allowed donations of almost enough insulin to cover patients.
This free insulin is a great outcome. However, the situation is still stressful because the clinic must rely on and anxiously await each shipment of insulin. Sometimes there is shortfall between batches where there isn’t enough insulin. The team came up with a great solution, involving the patients every step of the way. They called each patient to ask if they would be willing pay 200 shillings per vial which would allow the clinic to buy insulin direct from pharmacy to cover any shortfall. Anyone who couldn’t afford the 200 was still covered for free, but others who could pay were happy to do so because of the hugely subsidized rate and the ability to have continuous insulin.
We saw a lot of these types of innovative solutions by the team so that they could make the most of the resources available. One such solution was an insulin storage pot. Many Kenyans don’t have refrigerators but people with diabetes still need to keep their insulin cool, especially in the hot summer months. The solution pictured here keeps insulin cool by putting charcoal (or sand) in a clay pot with a glass jar inside of that to keep the insulin dry.
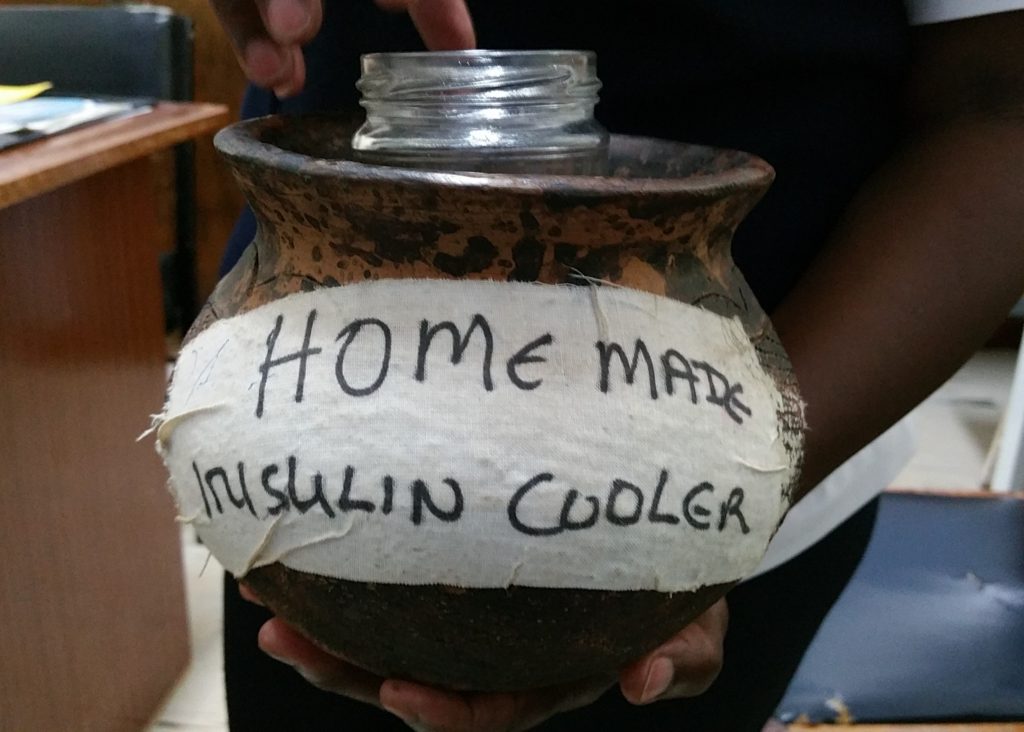
The team in Eldoret even has several people with type 1 diabetes on staff. We were happy to chat with Sam and Sheila who were diagnosed at age 16 and 13, respectively. They both had a hard time coping but now can support patients going through the same thing. Just as in the UK, teens can take a diabetes diagnosis particularly rough so it’s great for the patients to have doctors that fully understand the challenges.
Stigma is also a big issue in Kenya. Sheila, the social worker with type 1 diabetes, has a 4 yr old son so she is able to show that type 1 doesn’t prevent you from having a family. She works with financial aspect of diabetes care to help families find solutions to costly supplies and helps get the whole family involved in diabetes care.
The team hopes to hold type 1 camps or meet ups, especially for teens, and we want to support them in this. They also hope for more government support so that no child should die of diabetes in Kenya. We look forward to continuing to work with the team to advocate for better access for everyone with diabetes.





